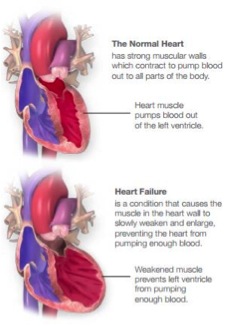
If you have heart failure, you’re not alone. About 5.7 million Americans are living with it today. In fact, it’s one of the most common reasons people age 65 and older go into the hospital. It can take years for heart failure to develop. Heart failure is called congestive heart failure when fluid builds up in various parts of the body. So if you don’t yet have it but are at risk for it, you should make lifestyle changes now to prevent it! Heart failure symptoms usually develop over weeks and months as your heart becomes weaker and less able to pump the blood that your body needs. Heart failure usually results in an enlarged heart (left ventricle).
Does your heart stop?
When you have heart failure, it doesn’t mean that your heart has stopped beating. It means that your heart isn’t pumping blood as it should. The heart keeps working, but the body’s need for blood and oxygen isn’t being met. Heart failure can get worse if it’s not treated. It’s very important to do what your doctor tells you to do. When you make healthy changes, you can feel a lot better and enjoy life much more!
Does your heart stop?
When you have heart failure, it doesn’t mean that your heart has stopped beating. It means that your heart isn’t pumping blood as it should. The heart keeps working, but the body’s need for blood and oxygen isn’t being met. Heart failure can get worse if it’s not treated. It’s very important to do what your doctor tells you to do. When you make healthy changes, you can feel a lot better and enjoy life much more!
What can happen?
Your heart does not pump enough blood.
Blood backs up in your veins.
Fluid builds up, causing swelling in your feet, ankles and legs. This is called “edema.”
Your body holds too much fluid.
Fluid builds up in your lungs. This is called “pulmonary congestion.”
Your body does not get enough blood, food and oxygen.
What are the signs of heart failure?
Shortness of breath, especially when lying down
Tired, run-down feeling
Coughing or wheezing, especially when you exercise or lie down
Swelling in feet, ankles and legs
Weight gain from fluid buildup
Confusion or can’t think clearly
How is it treated?
Your doctor may give you medicine to strengthen your heart and water pills to help your body get rid of excess fluids.
Your doctor will recommend a low-sodium (salt) diet.
You may be provided oxygen for use at home.
Your doctor may recommend certain lifestyle changes.
Surgery or cardiac devices may be needed, in some cases
Your heart does not pump enough blood.
Blood backs up in your veins.
Fluid builds up, causing swelling in your feet, ankles and legs. This is called “edema.”
Your body holds too much fluid.
Fluid builds up in your lungs. This is called “pulmonary congestion.”
Your body does not get enough blood, food and oxygen.
What are the signs of heart failure?
Shortness of breath, especially when lying down
Tired, run-down feeling
Coughing or wheezing, especially when you exercise or lie down
Swelling in feet, ankles and legs
Weight gain from fluid buildup
Confusion or can’t think clearly
How is it treated?
Your doctor may give you medicine to strengthen your heart and water pills to help your body get rid of excess fluids.
Your doctor will recommend a low-sodium (salt) diet.
You may be provided oxygen for use at home.
Your doctor may recommend certain lifestyle changes.
Surgery or cardiac devices may be needed, in some cases
What are the causes?
Past heart attack has done some damage to the heart muscle
Heart defects present since birth
High blood pressure
Heart valve disease
Diseases of the heart muscle
Infection of the heart and/or heart valves
Abnormal heart rhythm (arrhythmias)
Being overweight
Diabetes
Thyroid problems
Alcohol or drug abuse
Certain types of chemotherapy
Past heart attack has done some damage to the heart muscle
Heart defects present since birth
High blood pressure
Heart valve disease
Diseases of the heart muscle
Infection of the heart and/or heart valves
Abnormal heart rhythm (arrhythmias)
Being overweight
Diabetes
Thyroid problems
Alcohol or drug abuse
Certain types of chemotherapy
Cardiac Specialty Care
• Structural Heart Disease
• TAVR
• CardioMEMS (Heart Failure)
• PFO Closure
• TAVR
• CardioMEMS (Heart Failure)
• PFO Closure
• Coronary Intervention
• Complex Higher-Risk (And Indicated) Patients (CHIP) Angioplasty
• Atherectomy
• Impella and ECMO Support
• Complex Higher-Risk (And Indicated) Patients (CHIP) Angioplasty
• Atherectomy
• Impella and ECMO Support
• Peripheral Angioplasty
• Varicose Vein Treatment (Venous Ablation)
• DVT thrombectomy - IVC filter
• Carotid Stenting
• Varicose Vein Treatment (Venous Ablation)
• DVT thrombectomy - IVC filter
• Carotid Stenting
• Rhythm Management
• Pacemaker
• Holter Monitoring
• Exercise Stress Test
• Echocardiography
• Nuclear Stress Test
• Enhanced External Counterpulsation (EECP)
• Pacemaker
• Holter Monitoring
• Exercise Stress Test
• Echocardiography
• Nuclear Stress Test
• Enhanced External Counterpulsation (EECP)
